Perfect B, Doral Fl. | 02.12.26 | 5 min read.
Menopause can feel like a second puberty in women. Your body composition shifts, cravings change, sleep gets lighter, and suddenly the same routine does not work the way it used to. For many patients, the experience is best described as hormonal imbalance weight gain, and it can feel confusing because the rules you relied on for years stop delivering results.
This guide is designed to help you make a clinic style decision about hormonal imbalance weight gain in midlife. It explains what GLP 1 therapy can do, what it cannot do, what the evidence suggests for peri menopause and menopause, and how to protect muscle and long term results.
➔ Discover how our personalized weight loss treatment plan leverages these biological breakthroughs.
Quick answer: when GLP 1 therapy is and is not the right tool
GLP 1 therapy can be a strong option when menopause weight gain is tied to insulin resistance, appetite dysregulation, visceral fat gain, or repeated plateaus despite consistent habits. Many patients seeking help for hormonal imbalance weight gain are not looking for a shortcut. They are looking for a tool that makes a healthy plan possible again.
If you want a step by step menopause weight loss plan that combines GLP 1 therapy with nutrition and strength training, visit our [Weight Loss Treatment Plan Page].
GLP 1 may not be the best first step if you are experiencing red flag bleeding patterns, such as perimenopause bleeding for 3 weeks, or if the main issue is untreated sleep disruption, thyroid dysfunction, medication related weight gain, or unmanaged stress physiology. In those cases, the safest plan is to clarify the cause first.
The Perfect B difference: safe weight loss starts with systems, not hype
At Perfect B, we treat hormonal imbalance weight gain as a medical and body composition problem, not a willpower problem. Every protocol begins with baseline labs to assess metabolic health, liver and kidney function, glucose regulation, and nutritional status. Then we follow the data with regular check ins to track symptoms, weight loss curves, and body composition over time. This allows us to adjust early and avoid the common pattern of fast loss followed by burnout or rebound.
Because rapid fat loss increases nutrient demands, we often layer support thoughtfully, protein targets, electrolytes, and key micronutrients. This is one reason our patients do not only lose weight, they keep function and energy while they do it.
Why menopause weight gain feels different and why hormonal imbalance matters
What weight gain from hormonal imbalance means in real life
What weight gain from hormonal imbalance means in real life
Menopause related weight change is not just more calories. For many people it shows up as weight gain from hormonal imbalance. Shifting estrogen levels affect where fat is stored. Aging and stress can affect sleep, hunger signals, and energy expenditure. This is why the scale can rise even when your routine has not changed.
If you are looking for a clinic style evaluation of hormonal imbalance weight gain, including common questions about estrogen weight loss and timing in peri menopause, see our [Menopause Weight Gain Consultation Page].
During the transition, you may also notice perimenopause and irregular periods. This pattern can include skipped cycles, shorter cycles, or unpredictable bleeding, and it often overlaps with other symptoms that affect weight, such as sleep disruption and mood changes.
The big clinical point is that hormonal imbalance weight gain is not only about appearance. It is about metabolic health, inflammation, and long term function. That is why protecting lean mass matters as much as losing fat.
What GLP 1 therapy is and what it does in the body
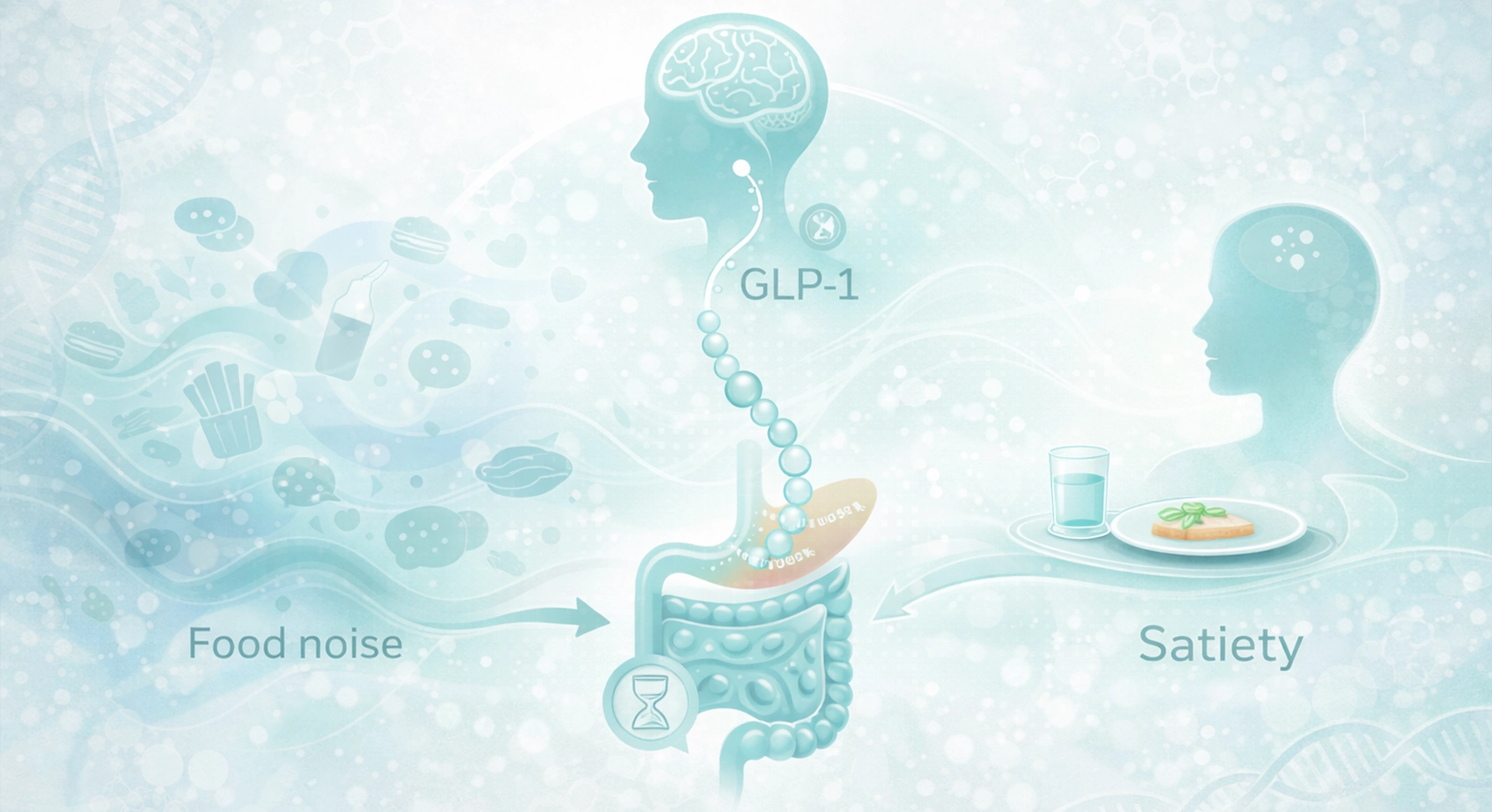
GLP 1 mechanism in plain language
GLP 1 medications mimic a gut hormone involved in fullness and blood sugar regulation. In practical terms, they can help you feel satisfied sooner, reduce food noise, and improve metabolic parameters for some patients. This has made GLP 1 therapy a major tool in modern weight management.
GLP 1 and hormone therapy: what is promising and what is individualized
Many menopause focused discussions also explore pairing GLP 1 medications with hormone therapy. Some reporting suggests that combining a GLP 1 medication with hormone therapy may produce greater weight loss than a GLP 1 medication alone. This is promising, but it is not a blanket rule. A clinician should individualize based on symptoms, risk profile, and goals.
How we think about rebalance hormones for weight loss in a clinic setting
This is also where readers often search for ways to rebalance hormones for weight loss. In a clinic setting, that phrase means evaluating the drivers behind weight change and symptoms, then building a plan that may include lifestyle interventions, targeted medical therapy, and careful follow up. If you are trying to rebalance hormones for weight loss, the safest path is a personalized assessment, not a one size fits all protocol.
➔ Learn more about financial options and consultations for regenerative medicine and weight loss.
Evidence snapshot: what research suggests in peri menopause and menopause

If you want a quick decision tool before you schedule, use our [GLP 1 Eligibility and Safety Checklist] to review candidacy, contraindications, and the questions to bring to your appointment.
A NewYork Presbyterian and Weill Cornell clinical summary describes a secondary analysis of SURMOUNT trial data evaluating tirzepatide in women across pre menopause, peri menopause, and post menopause stages. It reports meaningful reductions in body weight and waist measures regardless of reproductive stage.
How to use this in a clinic decision: this supports a key reassurance. GLP 1 class medications can still work during menopause. But it does not answer every real world question patients care about, like long term maintenance, muscle protection, and what happens after discontinuation.
➔ Check which options in our weight loss treatment plan might best fit your goals.
What many blogs skip: research gaps and real world risks, especially in perimenopause
RAND highlights a crucial point. Perimenopausal women are using GLP 1 medications, but this population has been underrepresented in research on unique risks and benefits. That can lead to decisions made with incomplete information.
Body composition: protect muscle and bone
GLP 1 medications can reduce weight, but how that weight is divided between fat and lean tissue matters. This is especially important during a life stage already associated with vulnerability in muscle and bone. For patients dealing with hormonal imbalance weight gain, a plan that ignores muscle can backfire.
Discontinuation and weight regain: plan long term
Weight maintenance after stopping therapy is a known concern. A good plan is not only how to lose. It is also how to keep. This is where nutrition strategy, strength training, and follow up matter.
Psychosocial dimension: visible change can have emotional impacts
Weight change is visible. Social feedback can be intense. Stigma, identity shifts, and distress around regain deserve clinical attention, not just the number on the scale.
Side effects and how clinics reduce drop off
Common side effects and comfort strategies
Common issues include nausea, constipation, reduced appetite, and tolerability challenges. A practical plan can improve comfort and adherence.
Tolerance and plateaus: how Perfect B stays ahead
At Perfect B, tolerance and plateaus are handled proactively. We adjust doses slowly, use pauses strategically when needed, and evaluate whether appetite suppression is causing unintended under nutrition. This matters for hormonal imbalance weight gain because midlife weight loss is only a win if it protects muscle and long term health.
A clinic ready protocol often includes:
- Baseline labs and body composition goals, not scale only
- Food strategy, especially protein
- Hydration and electrolytes to support comfort and adherence
- Resistance training plan
- Follow ups to adjust dose and tolerability and to keep adherence sustainable
Appearance and body composition: looking healthier, not simply thinner
Weight loss also affects how the body looks and feels, not just what the scale says. As fat volume decreases, some patients notice skin laxity or facial volume loss. Perfect B coordinates peptide protocols with regenerative and aesthetic treatments such as collagen stimulating therapies and volume support so patients look healthier, not simply thinner.
Are GLP 1 medications the same as weight loss peptides
Why people search peptides for fat loss when they mean GLP 1
Your keyword list shows a real pattern. Many people search GLP 1 medications through the lens of peptides to lose weight, peptides for losing weight, and peptides for fat loss. GLP 1 medications are peptide based therapies, but online searches often lump together very different things.
➔ If you are comparing peptide injections for weight loss with prescription GLP 1 options, read our peptides for Weight Loss Explained guide to understand what is evidence based, what is unregulated, and what safety screening should include.
Are peptides safe for weight loss? Safety lives in the details
How Perfect B selects peptides for fat loss safely
Peptides can be safe and effective for weight loss, but safety depends on careful selection, screening, and monitoring. At Perfect B, we prioritize evidence backed options, including GLP based therapies when appropriate, metabolism supportive peptides, and muscle preserving compounds, always matched to the individual.
When GLP 1 is not an option: alternatives that still move the needle
For patients with contraindications, we design personalized plans using non GLP peptides, metabolic support strategies, or regenerative approaches that still move the needle safely. This is another reason the question peptides for fat loss has to be answered with clinical context. Peptides for fat loss should never be a one size fits all approach.
To keep this clear, here is the clinic distinction:
- Weight loss peptides can refer to prescription GLP 1 medications, research peptides, or non validated fat loss products
- Peptides therapy may be used loosely in marketing. Clinically, it should mean a supervised, evidence based treatment plan
When people search peptides for fat loss, they may be looking for a single best solution. In reality, peptides for fat loss only make sense when the diagnosis, risks, and expectations are clear. The phrase peptides for fat loss can also appear next to claims like best fat burning peptide, best peptides for weight loss, best peptides for fat loss, and fat burner peptides. Those are usually consumer shorthand, not medical categories.
You will also see interest in oral peptides for weight loss and peptide injections for weight loss. In a clinic blog, the safest approach is to explain what is prescription based, what is evidence supported, what is unregulated, and what safety screening should look like.
If someone asks, what are peptides for weight loss, clarify that GLP 1 medications are among the best studied peptide style options in mainstream medicine. But best still depends on eligibility, goals, side effects, and long term plan.
A practical way to think about it is this. If your goal is peptides for fat loss, the best path is not hunting for a brand name. The best path is choosing a medical plan that manages appetite, protects muscle, and supports maintenance.
Who is a good candidate and what hormone rebalancing actually means
What a menopause weight gain evaluation should include
Many readers search for a hormone balancing weight loss supplement or ways to rebalance hormones for weight loss. People want a root cause solution. A helpful clinic response is to acknowledge the intent without overpromising.
In practice, a responsible approach looks like:
- Clarify whether weight change is primarily metabolic or driven by sleep disruption, thyroid issues, mood, medications, or eating patterns
- Consider whether hormonal treatment to lose weight, or broader hormonal weight loss treatment, is appropriate. This may mean evaluating menopause symptoms and risks, not hormones for everyone
- If GLP 1 is used, pair it with muscle protective behaviors and a maintenance strategy from day one
For many patients, the goal is to rebalance hormones for weight loss while also stabilizing energy, cravings, and sleep. That is reasonable, but it requires clarity. If you are trying to rebalance hormones for weight loss, we recommend tracking symptoms for two to four weeks and bringing that data to your clinician.
Integrating metabolic care with regenerative and aesthetic support
At Perfect B, we also treat appearance and tissue quality as part of health. When hormonal imbalance weight gain improves and fat volume drops, some people want support for skin quality and facial balance. We coordinate weight loss protocols with regenerative and aesthetic options, such as collagen stimulating therapies, to maintain a refreshed and healthy look.
This is also where weight gain from hormonal imbalance shows up as a lived experience. People often report they are doing everything right but still gaining, which is why hormonal imbalance weight gain becomes the primary complaint.
➔ If you want a guided plan that aligns GLP 1 treatment with menopause care and long term maintenance, see our Menopause Metabolic Program page.
Frequently Asked Questions (FAQ)
Q1: Perimenopause and irregular periods: what is common
Perimenopause and irregular periods are common as hormones fluctuate. Perimenopause and irregular periods can include skipped cycles, shorter cycles, or unpredictable bleeding. If bleeding is heavy, frequent, or new, get evaluated.
Q2: Irregular periods and perimenopause and irregular cycles perimenopause
Many people search irregular periods and perimenopause and irregular cycles perimenopause to describe the same issue. Track timing, flow, and symptoms. Bring that tracking to your visit, especially if symptoms are changing quickly.
Q3: Spotting in perimenopause: should I worry
Spotting in perimenopause can happen, but it is worth flagging if it is new, frequent, or heavy. Many people search perimenopause and spotting between periods, perimenopause spotting between periods, and spotting perimenopause. These patterns deserve context and sometimes medical evaluation.
Q4: Heavy periods in perimenopause or perimenopause bleeding for 3 weeks: when to call
If you have heavy periods in perimenopause, prolonged bleeding like perimenopause bleeding for 3 weeks, dizziness, anemia symptoms, or clotting, get evaluated promptly.
Q5: Night sweats before period: are these signs perimenopause is ending
Night sweats before period can be a perimenopause symptom, but not always a final stage marker. People search signs of end of perimenopause and signs perimenopause is ending, but symptom patterns vary.
Q6: Period late perimenopause: menstruation late for 2 days vs 2 weeks late menstruation
A period late perimenopause can be normal. But menstruation late for 2 days and 2 weeks late menstruation should be interpreted in context, including the possibility of perimenopause or pregnancy. Yes, can perimenopause woman get pregnant. Ovulation can still occur unpredictably.
Q6: Why am I not ovulating but having periods
In perimenopause, you can have bleeding that does not reflect a typical ovulatory cycle. This is why people ask why am i not ovulating but having periods and search period without ovulation signs. If you are trying to conceive or worried about abnormal bleeding, seek medical guidance.
Q6: Period during perimenopause: what patterns are common
A period during perimenopause may change in flow, frequency, and symptoms. Track patterns, including dates, flow, and spotting, and share them with your clinician.
Take Control of Your Hunger Today
GLP 1 therapy can be the right tool for menopause weight gain, but the best results come when it is used as part of a complete plan. Evidence aware prescribing, muscle protection, a long term maintenance strategy, and support for the psychosocial side of weight change all matter.
For many patients, the decision starts with naming the problem correctly. Hormonal imbalance weight gain is not a personal failure. It is a physiologic transition. If you are experiencing hormonal imbalance weight gain, or weight gain from hormonal imbalance, you deserve a plan built for midlife.
If you are considering GLP 1 therapy, bring three things to your consultation. Your symptoms, including perimenopause and irregular periods. Your goals, including scale and non scale goals. And your questions about long term maintenance. That is where the right tool becomes the right outcome.
Ready to optimize your health?
If you want to align appetite control with broader health goals, explore our Regenerative Medicine page to see how metabolic support and recovery focused care can complement a weight management strategy